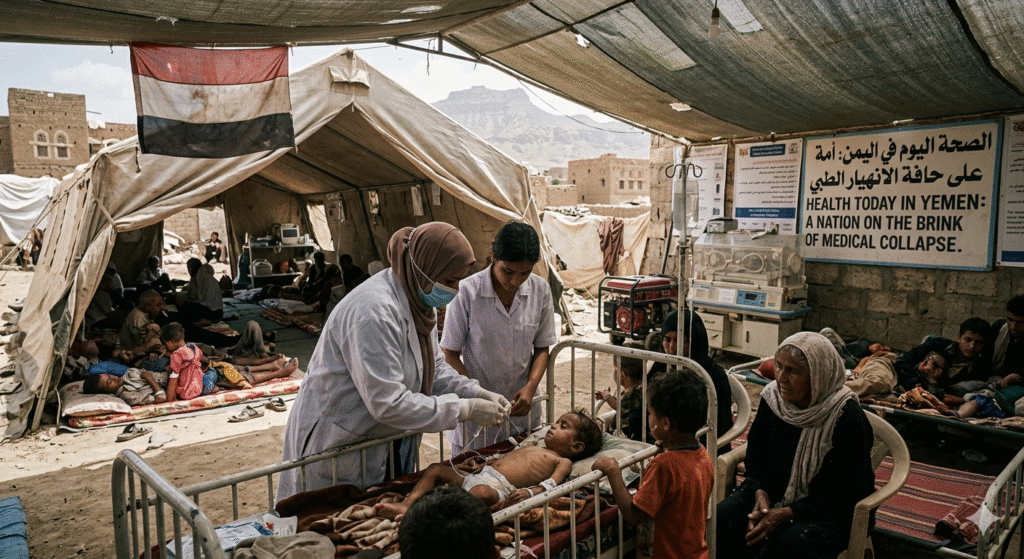
SANA’A/ADEN – In the spring of 2026, Yemen’s healthcare system is barely breathing. After more than a decade of civil war, economic collapse, and now crippling funding shortages, the country that was once the Arabian Peninsula’s most promising nation has become the site of the world’s most complex health emergency. With 22 million people – over two-thirds of the population – requiring humanitarian assistance, Yemen’s health crisis is not looming. It is here .
Part 1: The Funding Collapse – 70% of Facilities at Risk
The most immediate threat to Yemen’s health system is not bullets or bombs, but empty bank accounts. The Minister of Public Health and Population in Yemen’s caretaker government, Qasim Buhaibeh, issued a stark warning in early 2026: approximately 70% of health facilities are at risk of shutting down due to a sharp decline in donor funding, with decreases reaching 100% in some cases .
The numbers tell the story of collapse. Before the financial crisis, 60% of Yemen’s approximately 5,000 health facilities were functional. Today, that figure has dropped to 50% . If the funding decline continues, operational capacity could plummet to just 30% . The World Health Organization (WHO) has appealed for US$ 38.8 million to deliver emergency health assistance to 10.5 million people in 2026 – but even that represents a fraction of what is needed .
As one UN official put it: “Without sustained and timely funding, preventable diseases will spread unchecked, health facilities will be forced to scale down services, and the most vulnerable communities will pay the highest price” .
Part 2: The Cholera Resurgence – 1,626 New Cases and Counting
Cholera has returned to Yemen with a vengeance. According to the European Centre for Disease Prevention and Control, between late December 2025 and early February 2026, Yemen reported 1,626 new cholera cases, including one confirmed death . This represents a significant resurgence compared to earlier periods, though still below the catastrophic peaks of previous years.
The disease is a direct consequence of collapsing infrastructure. After years of war, water and sewage systems have been systematically damaged. In many areas, there is no clean drinking water. People are forced to consume contaminated supplies, and cholera spreads like wildfire through communities already weakened by malnutrition .
The WHO has documented that Yemen continues to experience “multiple, concurrent disease outbreaks” – cholera, measles, dengue fever, and polio – driven by low immunization coverage, unsafe water and sanitation, population displacement, and limited access to care . Climate-related shocks, including floods and extreme weather, are intensifying transmission risks and damaging already fragile health infrastructure .
Part 3: Malnutrition – A Generation Starving
Perhaps no statistic captures Yemen’s health catastrophe more starkly than child malnutrition. The numbers are staggering:
- 2.2 million children under five are acutely malnourished
- 516,000 children suffer from severe acute malnutrition (SAM) – the most dangerous form
- An additional 1.3 million pregnant and breastfeeding women are malnourished
In government-controlled areas alone, the number of children suffering from acute malnutrition rose by 34% compared to the previous year . The Integrated Food Security Phase Classification (IPC) Technical Working Group projects that all 117 surveyed districts in southern Yemen will experience “serious” levels of malnutrition or worse during the lean season from July to October .
The drivers of this crisis are multiple: disease outbreaks including cholera and malaria, high food insecurity, and limited access to safe drinking water. For a child already weakened by hunger, a bout of diarrhea from contaminated water can be a death sentence .
Part 4: The Vaccine Gap – Preventable Diseases Return
Yemen’s vaccination coverage has collapsed to just 63% complete coverage . This leaves millions of children vulnerable to diseases that were once nearly eradicated. According to Minister Buhaibeh, outbreaks of vaccine-preventable diseases – measles, polio, and diphtheria – have emerged due to the decline in free vaccination programs .
The consequences are unfolding in real-time. When a child contracts measles in Yemen today, the likelihood of survival depends on whether there is a functioning health facility within reach – and whether that facility has supplies, staff, and electricity. Too often, the answer to all three is no.
Part 5: Maternal Mortality – Women Dying in Childbirth
For pregnant women in Yemen, giving birth is a gamble with death. The maternal mortality rate has reached 183 deaths per 100,000 live births . To put this in perspective, this is approximately five times higher than the rate in neighboring Saudi Arabia and more than ten times higher than in developed countries.
Each death represents a family shattered, children left motherless, and a community losing one of its most vital members. The causes are predictable: lack of skilled birth attendants, absence of emergency obstetric care, chronic malnutrition, and the sheer physical toll of living through years of war and displacement.
Part 6: The Brain Drain – Doctors Fleeing a Dying System
Even where health facilities remain open, there are often no doctors to staff them. Minister Buhaibeh has highlighted a critical “brain drain” of medical personnel moving abroad or to the private sector due to weak incentives in the public sector and a hiring freeze that has lasted over a decade .
Yemen’s doctors and nurses are among the most resilient in the world. Many have worked without pay for months, improvising treatments when supplies run out, and risking their own lives to treat patients. But resilience has limits. As one health worker told a visiting journalist: “I love my country. But I cannot feed my children on love.” The exodus of trained medical personnel accelerates the collapse, creating a vicious cycle where remaining staff are overwhelmed, quality of care deteriorates, and more patients die.
Part 7: Chronic Disease Neglect – Cancer, Kidney Failure, and Heart Disease
The focus on infectious diseases and malnutrition often overshadows another crisis: the neglect of chronic conditions. According to the Ministry of Health, there has been a significant rise in cases of cancer, kidney failure, and heart disease across Yemen .
For a patient with kidney failure, regular dialysis is not a luxury – it is survival. But dialysis requires specialized equipment, sterile supplies, and consistent electricity – all of which are in short supply. Cancer patients face similar challenges: chemotherapy drugs are scarce, radiotherapy machines are broken or lack power, and palliative care is virtually non-existent.
These patients represent the “invisible” health crisis – the one that does not make headlines, but that slowly, relentlessly, claims lives every single day.
Part 8: The Humanitarian Response – A Race Against Time
Despite the overwhelming needs, the humanitarian community is not standing idle. The 2026 Yemen Humanitarian Needs and Response Plan (HNRP), published in March 2026, sets out a targeted response aiming to reach 12 million people – including 9.4 million prioritized for life-saving assistance based on severity .
The plan requests US$2.16 billion to deliver assistance at scale, including US$1.6 billion for prioritized life-saving interventions across sectors . As the UN Office for the Coordination of Humanitarian Affairs (OCHA) notes: “Humanitarian assistance saves lives. However, humanitarian action alone cannot reverse the drivers of Yemen’s crisis” .
On the ground, organizations like Qatar Charity have stepped in where possible. A recent three-month intervention supplied essential medicines, IV fluids, and medical consumables to 13 health facilities across Hudaydah, Hajjah, Taiz, and Aden, reaching approximately 48,000 people . The Director General of the Republican Hospital in Taiz confirmed that the support provided crucial relief for the facility, the city’s primary referral center for acute watery diarrhea cases .
Part 9: The WASH Crisis – No Clean Water, No Health
Health and water are inseparable. In Yemen, 14.4 million people require water, sanitation, and hygiene (WASH) assistance . Water scarcity and damaged infrastructure heighten both health and WASH vulnerabilities.
When people lack clean water, they cannot wash their hands. When they cannot wash their hands, diseases spread. When sewage systems are damaged, cholera and other waterborne diseases explode. The cycle is self-perpetuating and deadly. As one Red Cross official noted, the war has brought the health system “to the brink of collapse,” with cholera “only the most recent proof” of the utter devastation .
Part 10: The Vulnerable – Women, Children, IDPs, and the Muhamasheen
The health crisis does not affect all Yemenis equally. The 2026 HNRP explicitly identifies the most vulnerable groups: women and girls, persons with disabilities, internally displaced persons (IDPs), migrants, refugees, and the Muhamasheen – a marginalized community that has faced discrimination for generations .
There are 5.2 million IDPs in Yemen – people who have fled their homes, often multiple times, and now live in overcrowded camps with minimal sanitation, limited food, and no healthcare . For them, a simple respiratory infection can become pneumonia. A cut can become sepsis. A pregnancy can become a death sentence.
Women and girls face additional barriers: cultural restrictions on seeking care from male providers, lack of female health workers, and the specific health needs of pregnancy and childbirth in a system with no resources.
Part 11: The Funding Gap – $2.16 Billion Needed, Much Less Available
The 2026 HNRP’s request for $2.16 billion represents the minimum required to prevent mass death . But as of early 2026, funding remained critically short. The situation has been exacerbated by the global economic environment, as donor nations face their own budget pressures and competing humanitarian crises in Gaza, Sudan, and Ukraine.
Minister Buhaibe’s warning is unambiguous: “The weakness of external funding will ultimately hinder the ministry’s ability to provide basic services and double the escalating health risks” . He has called for urgent interventions and alternative funding models to prevent a potential public health catastrophe .
Part 12: The Path Forward – Beyond Humanitarian Aid
The humanitarian community in Yemen is advancing what it calls the “Global Humanitarian Reset” – a more people-centered, locally led, and cost-effective approach . The Humanitarian Country Team is committed to delivering assistance that prioritizes the most vulnerable while working with national and local institutions.
But as OCHA itself acknowledges, humanitarian action alone cannot solve Yemen’s crisis. “Reducing long-term needs will require joint efforts of all actors to restore essential services, revive livelihoods and strengthen resilience to future shocks, reinforced by progress towards a political solution” .
Without a political resolution to the conflict, without sustained investment in water infrastructure, without vaccination campaigns reaching every child, and without paying health workers a living wage, Yemen’s health system will continue to crumble. And millions of people will remain at risk of “deepening hunger, preventable illnesses and protection threats” .
Conclusion: A Predictable Catastrophe
What makes Yemen’s health crisis so devastating is that it is predictable and preventable. The drivers are understood: war, funding cuts, collapsed infrastructure, and a decade of neglect. The solutions are known: vaccines, clean water, trained staff, and functioning facilities.
Yet year after year, the funding falls short. Year after year, the conflict continues. And year after year, children die of diseases that should have been eradicated, mothers bleed to death in childbirth, and families watch helplessly as their loved ones suffer.
The WHO’s assessment is stark: “Yemen’s health system is stretched to its limits” . The question is not whether that system will break further. The question is whether the world will provide the resources to keep it from collapsing entirely. Without sustained support, millions of people will remain at risk – and for many, the next cough, the next fever, or the next bout of diarrhea will be their last.


